Skin Cancer
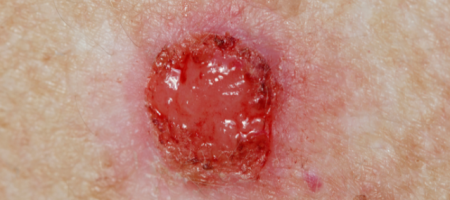
Skin cancer results from skin cells becoming damaged, most often by exposure to ultraviolet (UV) light from the sun or artificial sources like tanning beds.
Whenever we are exposed to UV light, the structure and function of our skin cells are affected. Over time this can lead to permanent cell damage, which will accumulate with each additional exposure. These damaged cells can turn into skin cancer.
Skin cancers are divided into melanoma (the most serious, potentially life-threatening skin cancer) and non-melanoma skin cancers. Squamous cell carcinomas (SCC) and basal cell carcinomas (BCC) are the most common non-melanoma skin cancers.
Symptoms
Early warning signs of skin cancer can vary; however, some crucial symptoms are listed below. If in doubt, check with your GP or dermatologist.
Melanomas are often pigmented lesions. Some clues to melanomas are by the ABCDE method.
A – Asymmetry
B – Border irregularity
C – Colour variation
D – Diameter (usually over 6mm)
E – Evolution (change and growing larger)
Skin cancers can also be pink, red or skin coloured. Skin cancers are commonly found on sun-exposed sites such as the face, scalp, ears, neck, upper chest and backs, outer arms and lower limbs. Important clues for skin cancer include:
- Change in size, shape or elevation
- Tenderness and/or pain
- Bleeding
- Sores or ulcers that do not heal within a few weeks, or which are recurrent.
If any of these occur, consult your GP or dermatologist as soon as possible. Your doctor may take a skin biopsy to confirm the diagnosis.
Causes
Other factors can impact the risk of skin cancer, but sun exposure is the leading cause. Less than 5% of melanomas are attributable to an inherited gene.
You are at a higher risk of skin cancer if:
- You previously had skin cancer.
- You have a family history of skin cancer.
- You have a skin type that burns quickly or is sensitive to UV light.
- You have had severe sunburns, particularly as a child.
- You actively tan, including the usage of solariums.
- You work outdoors.
- You are immune-suppressed, such as from immune-suppressive medications or have had an organ transplant
Treatments
Several different treatment methods are available for each form of skin cancer. The treatment method will depend on the type and severity of the skin cancer. Some common examples of available treatments are listed below.
Surgical excision
Surgical excision is the most common treatment for skin cancers. It is usually performed under local anaesthetic. The surgical wound is usually closed with skin sutures, leaving a scar. More extensive wounds may be closed using a skin graft or flap and may require general anaesthetic.
Cryotherapy
Cryotherapy involves freezing a skin lesion with liquid nitrogen. It is generally reserved for benign lesions like solar (actinic) keratoses but may be used for superficial skin cancers in some situations.
Curettage / Electrodessication
Curettage is a surgical technique where the skin lesion is scraped off the skin. It is used for superficial skin cancers and avoids the need for sutures. The curettage site usually heals with a white scar.
Mohs’ surgery
In Mohs’ surgery, the surgeon uses a microscope immediately following surgery to examine the skin that has been surgically excised to check that the tumour has been completely removed. It has the highest cure rate of all surgical treatments and aims to conserve as much normal skin as possible.
Mohs’ surgery is the treatment of choice for more complicated tumours, particularly on the face. This type of surgery is only available in certain centres.
Superficial Radiotherapy
Radiotherapy uses X-rays to destroy cancer cells and effectively treats some skin cancers.
Older age groups who are not suitable for surgery may benefit from this option.
Radiotherapy has the advantage of avoiding a surgical wound and can have an excellent cosmetic outcome in the short to medium term.
Fluorouracil cream
Fluorouracil cream is a chemotherapy cream that acts to kill off the damaged cells.
It is self-applied for up to a 4-week period. It causes a red, inflamed reaction in the treated area that recovers within weeks after the treatment is completed.
It is reserved for superficial skin cancers, not for melanoma or invasive SCC.
Imiquimod cream
Imiquimod is a cream that stimulates the immune system to destroy cancer cells. It is self-applied for up to a 6 week period.
Imiquimod causes a red, inflamed reaction and is reserved for specific types of superficial skin cancers, not melanoma or invasive SCC
PDT is a non-surgical treatment involving applying a light-sensitive chemical to the skin followed by illumination with a specialised light source.
PDT results in the selective destruction of cancer cells and avoids damage to the surrounding skin. An inflammatory reaction follows with redness, swelling and peeling, which typically heals with an excellent cosmetic result.
Like other non-surgical treatments, PDT must not be used for invasive SCCs or Melanoma.
Resources
For further information, you can visit the following resources:

