Occupational Contact Dermatitis
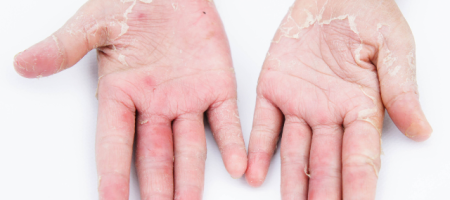
Occupational contact dermatitis (OCD) is a form of skin inflammation caused by contact with substances in the workplace. It can occur at any time of life, whether there is history of skin conditions or allergies or not.
Types
Irritant contact dermatitis
The most common form of OCD is irritant contact dermatitis. This is caused when an irritant contacts the skin for a sufficiently long enough time to damage the skin cells. Often there is exposure to multiple irritants at the same time. Wet work, with successive wetting and drying of the skin, is the most common cause of irritant contact dermatitis. People with a background of atopic eczema often have a more easily damaged skin barrier and are at increased risk of irritant contact dermatitis. Other causes of irritant contact dermatitis are harsh soaps, solvents, oils, and physical factors such as heat, sweating and friction. Once the skin barrier is damaged with irritant contact dermatitis, there is an increased risk of developing allergic contact dermatitis.
Allergic contact dermatitis
Allergic contact dermatitis occurs when an allergen penetrates the skin and combines with the skin immune cells. The allergen (sometimes referred to as the sensitiser) then moves to the lymph glands where they react with T-lymphocytes which produce cells which remember the particular allergen. The next time the allergen contacts the skin, this will result in a rash, known as allergic contact dermatitis. Only certain small chemicals have the capability to cause allergic contact dermatitis. Common occupational causes include rubber accelerators in rubber products, especially in protective gloves, preservatives in skincare products, workplace chemicals and paints, chromate in cement and leather, hairdressing chemicals and epoxy resins.
Contact urticaria
Contact urticaria is another form of allergy which happens almost immediately on skin contact with an allergen (usually within 10-30 minutes). It can cause hay fever-like symptoms or asthma, as well as skin reactions. Contact urticaria is diagnosed by skin prick-testing or a blood test. Common causes include latex, hairdressing bleach (ammonium persulphate) and some foods contacted by food handlers.
Occupations
The people who are most at risk are those in occupations performing wet work. Hairdressers, nurses, dentists, cleaners and mechanics are most commonly affected, and it is also very common in the healthcare industry.
Some chemicals cause allergic reactions that may result in more severe dermatitis. These especially include chromate in cement and epoxy resins, in glues and some floor finishings. Understanding which jobs are associated with occupational dermatitis is important, so people in these occupations can take extra precautions.
Symptoms
Occupational contact dermatitis is usually itchy. It commonly affects the hands and generally relates to the site of contact of the irritants and allergens. Affected skin may have any of the following features.
- Redness (erythema)
- Dryness or scaling
- Swelling (oedema)
- Blisters that are small (vesicles) or large (bullae)
- Cracks (fissuring)
- Lichenification (thickened, lined skin)
Treatments
The most important part of treatment is having an accurate diagnosis from a specialised dermatologist. This is achieved through a process of allergy testing called patch testing, whereby patients attend for 3 visits over 1 week. The Skin Health Institute is the national leader in patch testing. Tests are applied to the back and removed after 48 hours. These tests reproduce allergic reactions in the skin.
However, there is no test for irritant contact dermatitis, and this is often diagnosed after exclusion of allergic contact dermatitis, although these conditions may co-exist. In addition, patients may also have a component of endogenous skin disease, such as eczema or psoriasis.
Treatments for occupational dermatitis include:
- Avoidance of known allergens or irritants
- Appropriate skin protection: use of the right gloves for the job
- Moisturising creams
- Soap substitutes
- Topical corticosteroids
- Antibiotics if there is secondary infection
- Phototherapy (light therapy)
- Grenz rays (the Skin Health Institute has pioneered the use of Grenz rays, a superficial form of radiotherapy, to treat occupational hand dermatitis)
- Systemic therapy (oral tablets or injections) may occasionally be used in severe cases.
Resources
For further information, you can visit the following resources:

